320+ 5-Star Google Reviews
Google Reviews
Expert Lower Back Pain Treatment in Bee Cave, TX
Elite Wellness Chiropractic helps Bee Cave residents find lasting relief from lower back pain through evidence-based corrective care. Dr. Mikala Booher, DC, provides research-backed treatment protocols that address the root cause of your pain - not just the symptoms.
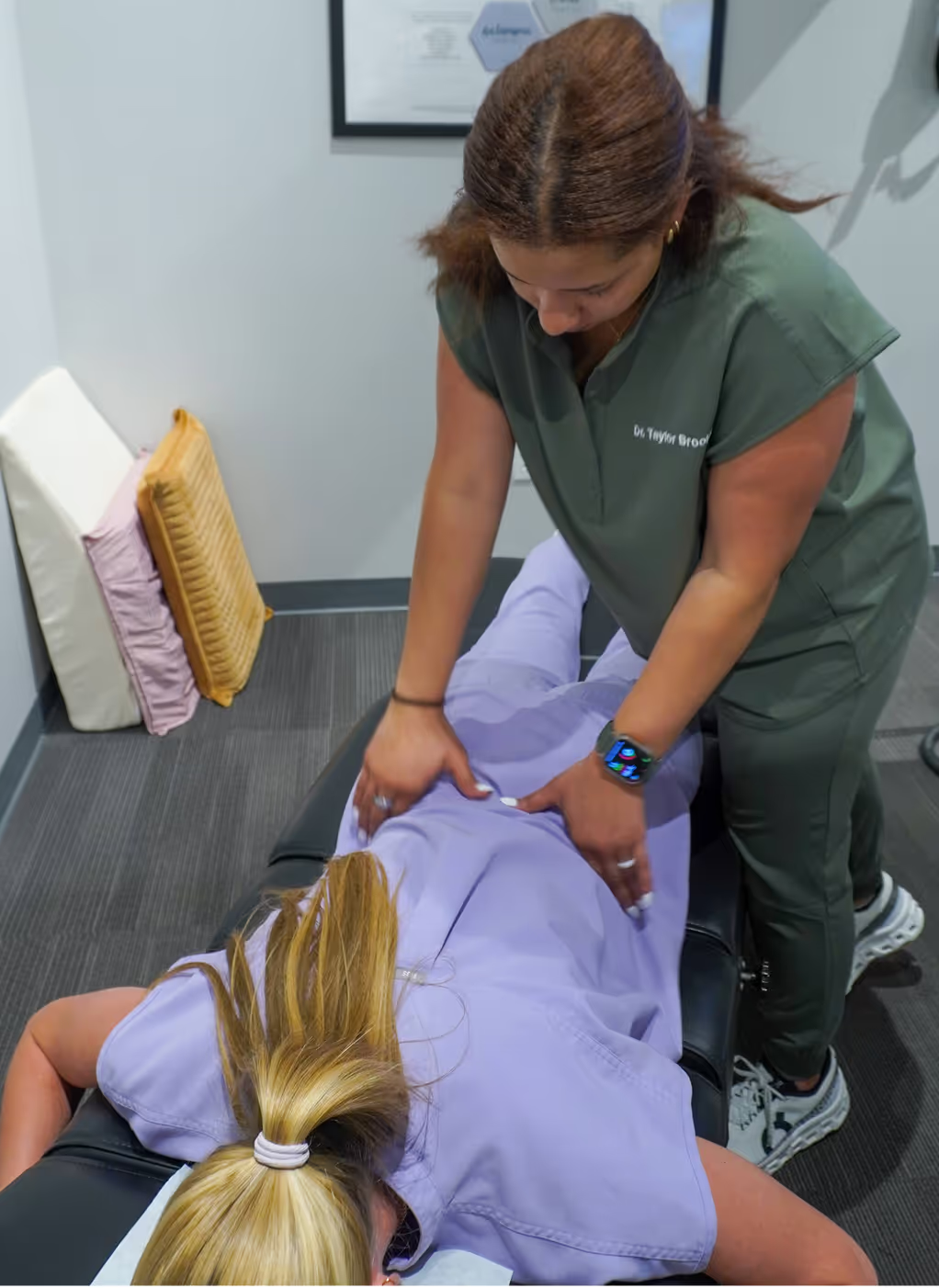
Key Takeaways: What You Need To Know About Lower Back Pain Treatment
- Evidence-backed relief: Spinal manipulation shows 50% patient improvement within 2 weeks; mean pain reduction of 9.95 points on a 100-point scale (Paige et al., 2017)
- Root cause identification: Lower back pain stems from mechanical dysfunction, including facet joint inflammation, disc degeneration, and muscle imbalances - not just "muscle strain.
- Decision logic for care: If back pain has persisted beyond 6 weeks or pain radiates below the knee, seek specialized chiropractic evaluation
- Treatment timeline: Clinical studies show optimal outcomes with 8-12 chiropractic treatments over 6 weeks for subacute cases
- Safety profile confirmed: Serious adverse events from spinal manipulation occur in only 1 per 1-2 million treatments - safer than many common medications
- Decision logic for care: If back pain has persisted beyond 6 weeks or pain radiates below the knee, seek specialized chiropractic evaluation
- Treatment timeline: Clinical studies show optimal outcomes with 8–12 chiropractic treatments over 6 weeks for subacute cases
- Safety profile confirmed: Serious adverse events from spinal manipulation occur in only 1 per 1–2 million treatments — safer than many common medications.
- Emergency warning: Bowel/bladder dysfunction, saddle numbness, or progressive leg weakness = seek emergency care immediately
Signs, Symptoms & When to Pay Attention to Your Lower Back Pain
Lower back pain isn't just 'something that happens with age' or a simple muscle strain. The research reveals a complex interplay of mechanical, neurological, and biomechanical factors that create the pain experience.

The Mechanical Breakdown Process
Facet joint dysfunction represents one primary pathway. These small joints become inflamed when exposed to repetitive stress, causing capsular irritation and local pain. Intervertebral disc degeneration follows a similar pattern, leading to altered biomechanics (Adams & Roughley, 2006).
The Neuromuscular Component
Research by Hodges & Richardson (1996) revealed that people with lower back pain develop specific muscle dysfunction patterns. The deep stabilizing muscles stop activating properly, leaving the spine vulnerable to further injury.
Central Sensitization
When lower back pain persists beyond 12 weeks, central sensitization mechanisms often develop (Woolf, 2011). The nervous system becomes hypersensitive, amplifying normal sensations into pain signals.
Signs, Symptoms & When to Pay Attention to Your Lower Back Pain
Mechanical Pain
- Dull, aching sensation across the lower back
- Stiffness after inactivity
- Worsens with forward bending
- Improves with position changes
- Localized muscle spasms
Radicular Pain
- Sharp, shooting pain intoleg
- Numbness/tingling along nerves
- Pain follows coughing/sneezing
- Weakness in specific muscle groups (foot drop)
Inflammatory Pattern
- Morning stiffness > 30 mins
- Improves with movement
- Worsens with rest
- Night pain disrupting sleep
Seek Immediate Emergency Care If
- Bowel or bladder dysfunction
- Saddle numbness (loss of sensation between legs)
- Progressive weakness in both legs
- Severe pain following significant trauma
- Fever accompanying back pain
Consider Chiropractic Evaluation If:
- Pain persisting beyond 6 weeks without improvement
- Recurring episodes becoming more frequent or severe
- Pain interfering with sleep or daily activities
- Numbness or tingling extending below the knee
- Difficulty with prolonged standing or walking
EVIDENCE-BASED OUTCOMES
What the Research Says About Chiropractic Care
of patients improve within 2 weeks
(Pengel et al., 2003)
mean pain reduction (100-pt scale)
(Paige et al., 2017)
treatments causes serious events
(Haldeman et al., 1999)

Landmark Clinical Trials
The UK BEAM trial (2004) in the BMJ, one of the largest randomized controlled trials in manual therapy, demonstrated superior outcomes for manipulation compared to usual care - a clinically meaningful difference maintained at 12-month follow-up.
Comparative Effectiveness
Cherkin et al. (1998) in the New England Journal of Medicine found both chiropractic care and McKenzie physical therapy demonstrated similar outcomes at 4-week follow-up, significantly superior to educational interventions alone.
Treatment Timeline Evidence
Hondras et al. (2009) demonstrated that 8-12 treatments over 6 weeks produces superior outcomes compared to shorter treatment courses for subacute and chronic presentations.
Expert Back Pain Chiropractor: Our Approach at Elite Wellness

Comprehensive Assessment Protocol
Thorough evaluation including history-taking, orthopedic testing, and movement analysis. On-site digital X-ray is utilized only when clinically indicated per ACP guidelines.
Evidence-Based Treatment
Manual chiropractic adjustment targeting specific segments. Low-force Activator Method available. Protocols follow the Flynn et al. (2002) clinical prediction rule.
Corrective Exercise Integration
Motor control retraining targeting deep stabilizing muscles (multifidus and transverse abdominis). Rehab begins during the first week of treatment.
Reassessment & Monitoring
Systematic reassessment at 2-week intervals using validated outcome measures. Less than 20% improvement triggers plan modification or referral.
Your Clear Path to Relief:
Our 3-Step Process
STEP 01
The Discovery
Comprehensive biomechanical exam + digital X-rays (if needed). Dr. Booher identifies the exact structural causes of your pain.
STEP 02
The Correction
Evidence-based spinal adjustments, manual therapy, and corrective protocols targeting your specific dysfunction patterns.
STEP 03
The Optimization
Motor control retraining, corrective exercises, and reassessment milestones. You leave with tools to maintain your results.
What to Expect During Treatment at Our Bee Cave Clinic
Initial Visit (60-90 mins)
- Comprehensive history-taking and pain pattern assessment
- Postural analysis + orthopedic and neurological testing
- Range of motion measurement with inclinometry
- Digital X-rays if clinically indicated
- First treatment typically begins the same day
Follow-up Visits (30-45 mins)
- Brief symptom tracking with the Numeric Rating Scale
- Targeted examination of previously restricted areas
- Progressive treatment advancing through healing phases
- Home care protocols and corrective exercises assigned
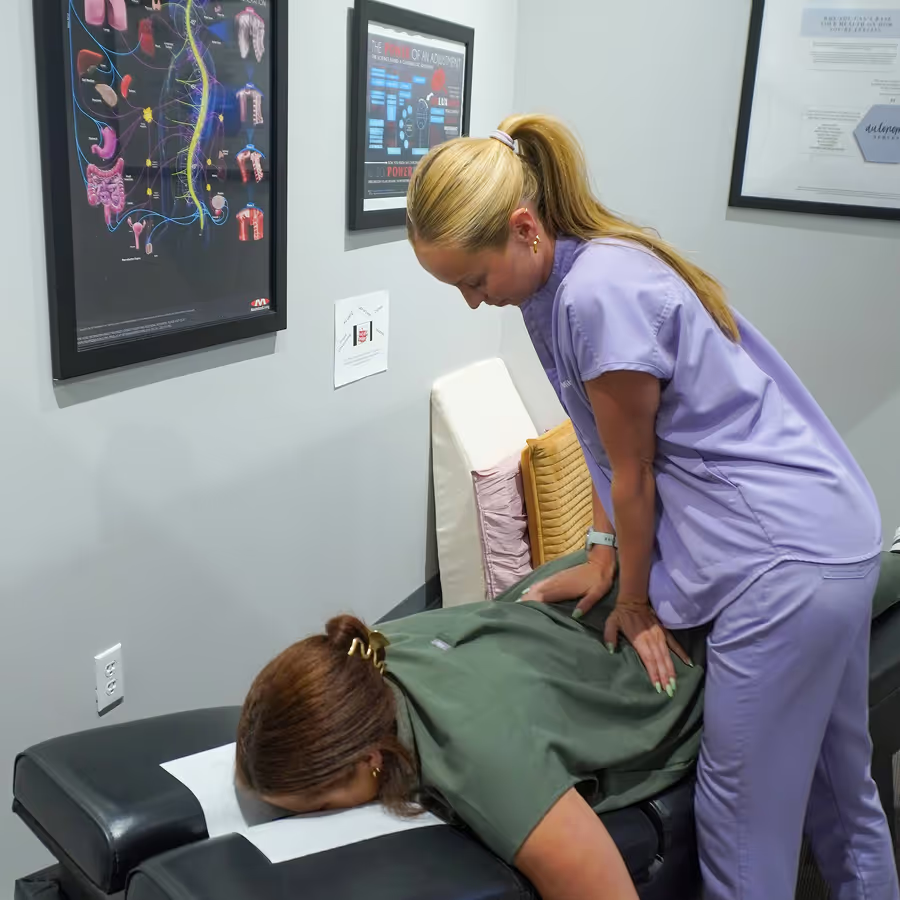
Common Questions About Back Pain & Chiropractic Care
Yes. Haldeman et al. (1999) documented serious adverse events occur in only 1 per 1–2 million spinal manipulations — significantly safer than many common medications. Minor soreness resolves within 24–48 hours. Dr. Booher performs thorough screening before every treatment.
Pengel et al. (2003) found 50% of acute patients improve within 2 weeks. The Paige et al. (2017) meta-analysis showed significant pain reduction averaging 9.95 points on a 100-point scale within 6 weeks. Dr. Booher reassesses every 2 weeks.
Cherkin et al. (1998) found equivalent results between chiropractic and McKenzie physical therapy at 4-week follow-up. Chiropractic emphasizes joint mobility through manual therapy; PT focuses on exercise retraining. Combined approaches often provide the best outcomes.
Acute (under 6 weeks): 6–8 sessions over 3–4 weeks. Subacute (6–12 weeks): 8–12 sessions over 6 weeks. Chronic: 12–16 sessions over 8–12 weeks. Progress reassessed every 6 treatments.
Yes, for many cases. Bronfort et al. (2008) demonstrated manual therapy effectiveness for stable or improving disc herniations. Large herniations with progressive neurological deficits may need medical management first. Dr. Booher performs careful neurological screening and refers when necessary.
Not routinely. ACP guidelines advise against imaging for nonspecific acute pain without red flag symptoms. Dr. Booher orders X-rays only when clinically indicated (suspected fractures, trauma, neurological deficits). On-site digital X-ray is available if needed.
Avoid prolonged sitting (move every 30 minutes), heavy lifting over 10–15 lbs initially, and activities that reproduce pain. Research recommends maintaining normal activity within pain tolerance — prolonged bed rest delays recovery.
Still have questions?
What Our Patients Say About Back Pain Relief
Sarah M.
Bee Cave, TX
"After 3 years of lower back pain, Dr. Booher found the problem in my first visit. Six weeks later I'm back to running and playing with my kids without pain."
James T.
Lakeway, TX
"I was skeptical of chiropractic care until I saw my X-rays. Now I understand WHY I was hurting. Finally getting real answers instead of just masking symptoms."
Michael R.
Westlake, TX
"Most chiropractors just adjusted me and sent me home. Dr. Booher gave me a whole corrective plan with exercises. Night and day difference in my recovery."
Related Conditions We Also Treat
Start Your Recovery Journey with Our Bee Cave Team
Don't let lower back pain control your life any longer. Research consistently demonstrates that early intervention produces the best outcomes. The longer you wait, the more likely your acute pain becomes chronic.
*Dr. Mikala Booher, DC serves Bee Cave, Lakeway, West Lake Hills, Dripping Springs, and Southwest Austin.
Adams, M. A., & Roughley, P. J. (2006). What is intervertebral disc degeneration, and what causes it? Spine, 31(18), 2151-2161.
Assendelft, W. J., Morton, S. C., Yu, E. I., Suttorp, M. J., & Shekelle, P. G. (2003). Spinal manipulative therapy for low back pain. Cochrane Database of Systematic Reviews, (1), CD000447.
Bogduk, N. (2005). Clinical anatomy of the lumbar spine and sacrum (4th ed.). Churchill Livingstone.
Bronfort, G., Haas, M., Evans, R. L., & Bouter, L. M. (2008). Efficacy of spinal manipulation and mobilization for low back pain and neck pain: a systematic review and best evidence synthesis. The Spine Journal, 8(3), 213-225.
Bronfort, G., Maiers, M. J., Evans, R. L., et al. (2011). Supervised exercise, spinal manipulation, and home exercise for chronic low back pain: a randomized clinical trial. Spine, 36(21), 1813-1824.
Bronfort, G., Maiers, M. J., Evans, R. L., et al. (2012). Supervised exercise, spinal manipulation, and home exercise for chronic low back pain: a randomized clinical trial. Annals of Internal Medicine, 156(2), 132-140.
Carey, T. S., Garrett, J., Jackman, A., et al. (1995). The outcomes and costs of care for acute low back pain among patients seen by primary care practitioners, chiropractors, and orthopedic surgeons. New England Journal of Medicine, 333(14), 913-917.
Cassidy, J. D., Boyle, E., Côté, P., et al. (2008). Risk of vertebrobasilar stroke and chiropractic care: results of a population-based case-control and case-crossover study. Spine, 33(4S), S176-S183.
Cherkin, D. C., Deyo, R. A., Battié, M., Street, J., & Barlow, W. (1998). A comparison of physical therapy, chiropractic manipulation, and provision of an educational booklet for the treatment of patients with low back pain. New England Journal of Medicine, 339(15), 1021-1029.
Childs, J. D., Fritz, J. M., Flynn, T. W., et al. (2004). A clinical prediction rule to identify patients with low back pain most likely to benefit from spinal manipulation: a validation study. Annals of Internal Medicine, 141(12), 920-928.
Chou, R., Qaseem, A., Snow, V., et al. (2007). Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society. Annals of Internal Medicine, 147(7), 478-491.
Coulter, I. D., Crawford, C., Hurwitz, E. L., et al. (2018). Manipulation and mobilization for treating chronic low back pain: a systematic review and meta-analysis. The Spine Journal, 18(6), 866-879.
Cramer, G. D., Tuck Jr, N. R., Knudsen, J. T., et al. (2000). Effects of side-posture positioning and side-posture adjusting on the lumbar zygapophysial joints as evaluated by magnetic resonance imaging: a before and after study with randomization. Journal of Manipulative and Physiological Therapeutics, 23(6), 380-394.
Deyo, R. A., & Diehl, A. K. (1988). Cancer as a cause of back pain: frequency, clinical presentation, and diagnostic strategies. Journal of General Internal Medicine, 3(3), 230-238.
Flynn, T., Fritz, J., Whitman, J., et al. (2002). A clinical prediction rule for classifying patients with low back pain who demonstrate short-term improvement with spinal manipulation. Spine, 27(24), 2835-2843.
Fritz, J. M., Childs, J. D., & Flynn, T. W. (2005). Pragmatic application of a clinical prediction rule in primary care to identify patients with low back pain with a good prognosis following a brief spinal manipulation intervention. BMC Family Practice, 6(1), 29.
Haas, M., Sharma, R., & Stano, M. (2005). Cost-effectiveness of medical and chiropractic care for acute and chronic low back pain. Journal of Manipulative and Physiological Therapeutics, 28(8), 555-563.
Haldeman, S., Kohlbeck, F. J., & McGregor, M. (1999). Risk factors and precipitating neck pain causing vertebrobasilar artery dissection after cervical trauma and spinal manipulation. Spine, 24(8), 785-794.
Hartvigsen, J., Hancock, M. J., Kongsted, A., et al. (2018). What low back pain is and why we need to pay attention. The Lancet, 391(10137), 2356-2367.
Hodges, P. W., & Richardson, C. A. (1996). Inefficient muscular stabilization of the lumbar spine associated with low back pain: a motor control evaluation of transversus abdominis. Spine, 21(22), 2640-2650.
Hondras, M. A., Long, C. R., Cao, Y., Rowell, R. M., & Meeker, W. C. (2009). A randomized controlled trial comparing 2 types of spinal manipulation and minimal conservative medical care for adults 55 years and older with subacute or chronic low back pain. Journal of Manipulative and Physiological Therapeutics, 32(5), 330-343.
Licciardone, J. C., Minotti, D. E., Gatchel, R. J., Kearns, C. M., & Singh, K. P. (2013). Osteopathic manual treatment and ultrasound therapy for chronic low back pain: a randomized controlled trial. Annals of Family Medicine, 11(2), 122-129.
Meade, T. W., Dyer, S., Browne, W., Townsend, J., & Frank, A. O. (1990). Low back pain of mechanical origin: randomised comparison of chiropractic and hospital outpatient treatment. BMJ, 300(6737), 1431-1437.
Paige, N. M., Miake-Lye, I. M., Booth, M. S., et al. (2017). Association of spinal manipulative therapy with clinical benefit and harm for acute low back pain: systematic review and meta-analysis. JAMA, 317(14), 1451-1460.
Pengel, L. H., Herbert, R. D., Maher, C. G., & Refshauge, K. M. (2003). Acute low back pain: systematic review of its prognosis. BMJ, 327(7410), 323.
Qaseem, A., Wilt, T. J., McLean, R. M., & Forciea, M. A. (2017). Noninvasive treatments for acute, subacute, and chronic low back pain: a clinical practice guideline from the American College of Physicians. Annals of Internal Medicine, 166(7), 514-530.
Rubinstein, S. M., Leboeuf-Yde, C., Knol, D. L., de Koekkoek, T. E., Pfeifle, C. E., & van Tulder, M. W. (2007). The benefits outweigh the risks for patients undergoing chiropractic care for neck pain: a prospective, multicenter, cohort study. Journal of Manipulative and Physiological Therapeutics, 30(6), 408-418.
Rubinstein, S. M., Terwee, C. B., Assendelft, W. J., de Boer, M. R., & van Tulder, M. W. (2012). Spinal manipulative therapy for acute low-back pain. Cochrane Database of Systematic Reviews, (9), CD008880.
Rubinstein, S. M., van Middelkoop, M., Assendelft, W. J., de Boer, M. R., & van Tulder, M. W. (2011). Spinal manipulative therapy for chronic low-back pain. Cochrane Database of Systematic Reviews, (2), CD008112.
UK BEAM Trial Team. (2004). United Kingdom back pain exercise and manipulation (UK BEAM) randomised trial: effectiveness of physical treatments for back pain in primary care. BMJ, 329(7479), 1377.
Woolf, C. J. (2011). Central sensitization: implications for the diagnosis and treatment of pain. Pain, 152(3), S2-S15.