320+ 5-Star Google Reviews
Google Reviews
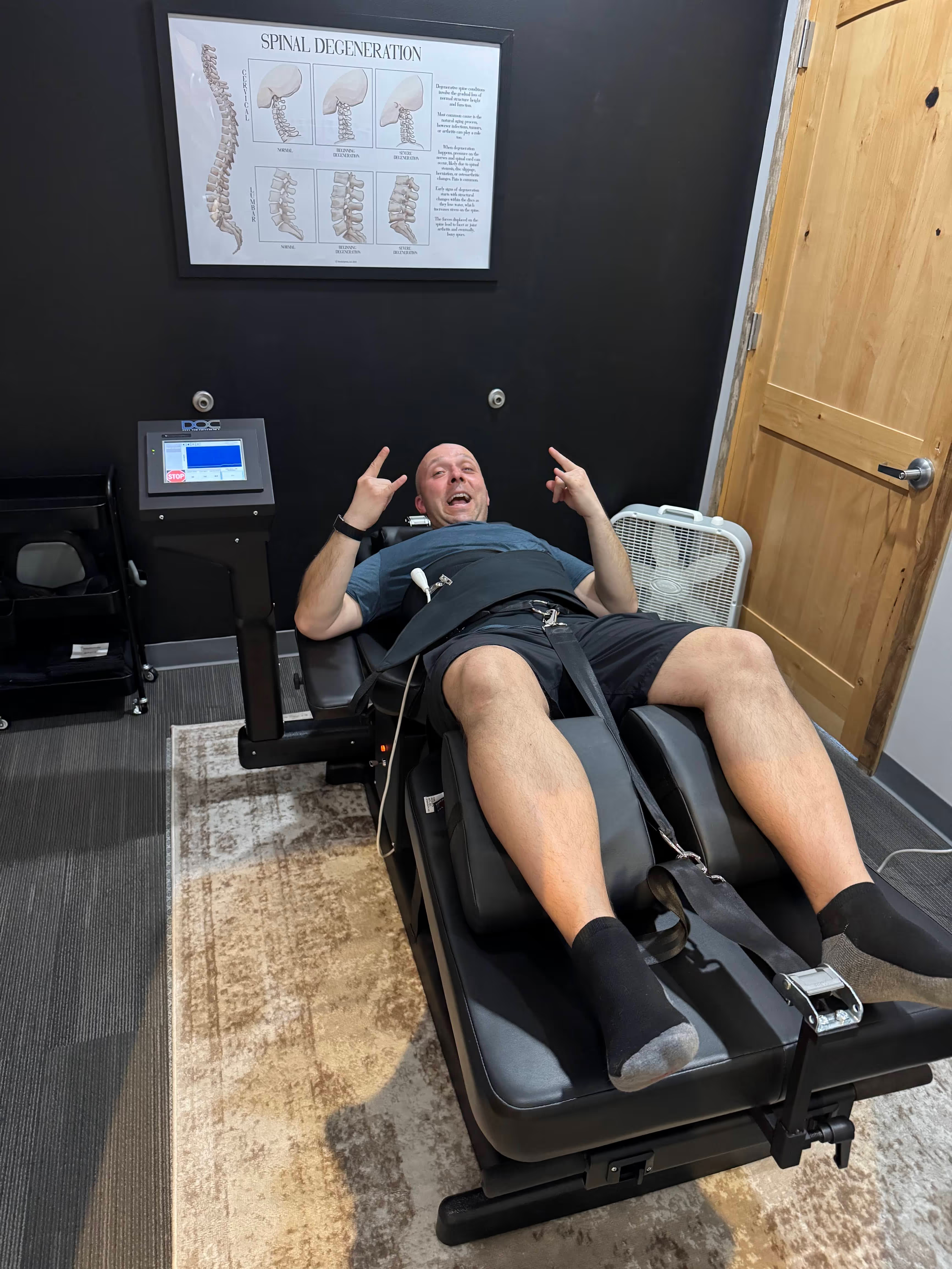
Non-Surgical Spinal Decompression in Bee Cave
Looking for targeted relief from herniated discs, sciatica, or spinal stenosis? We utilize the advanced DOC table and evidence-based corrective care protocols to bypass muscle guarding, achieve negative intradiscal pressure, and promote genuine healing without surgery.
Key Takeaways: What You Need To Know About Decompression
- Research-supported mechanism: Decompression creates negative intradiscal pressure (-100 to -200 mmHg), promoting retraction of herniated disc material and influx of nutrients essential for healing (Ramos & Martin, 1994).
- Clinical effectiveness: A systematic review found that 86% of patients with herniated or degenerative discs reported significant pain reduction, maintained at long-term follow-ups (Macario & Pergolizzi, 2006).
- Not the same as traction: True decompression uses variable force curves that bypass the body's protective muscle guarding reflex, achieving pressure changes that linear traction cannot replicate.
- Ideal candidates: Patients with MRI-confirmed herniated/bulging discs, degenerative disc disease, sciatica, or spinal stenosis who haven't responded to medication or physical therapy.
- Treatment timeline: Clinical protocols typically involve 12–24 sessions based on severity, with most patients reporting measurable symptom improvement within the first 4–6 sessions.
- Important contraindications: Not appropriate for patients who are pregnant, have severe osteoporosis, have prior spinal surgery with hardware, or have unstable spinal fractures.
Understanding Spinal Decompression - How It Works
Intervertebral discs function as hydraulic shock absorbers. When a disc herniates or bulges, it pushes outward, compressing adjacent nerve roots. Traditional treatments address pain but don't directly affect the disc itself.

The Core Mechanism: Negative Pressure
Controlled distraction forces create measurable negative pressure within the disc space. This draws herniated disc material back toward the center and creates an osmotic gradient that pulls water, oxygen, and nutrients into the disc for repair.
Why It's Not Simple Traction
Standard traction applies a constant pull, triggering the body's muscle guarding reflex. True decompression systems use logarithmic force curves that gradually increase and decrease tension in patterns the body cannot anticipate, bypassing this reflex entirely.
The DOC Table Advantage
Most tables are limited to linear pulling. Our DOC table offers supine or prone positioning, lateral flexion, and rotational decompression. This multi-planar capability allows us to target the specific angle of your disc herniation.
Conditions Treated - Is This Therapy Right For You?
Herniated & Bulging Discs
- Disc material extends beyond the normal boundary
- Often causes radiating pain (lumbar or cervical)
- Decompression creates negative pressure to retract material
Degenerative Disc Disease
- Progressive loss of disc height and hydration
- Often affects multiple levels (L4-L5, L5-S1)
- Decompression promotes vital nutrient diffusion
Sciatica & Spinal Stenosis
- Sharp, shooting pain radiating down the leg
- Narrowing of the spinal canal or neural foramina
- Opens foraminal spaces and reduces nerve compression
not appropriate if you have:
- Prior spinal surgery with hardware (rods, screws, cages)
- Pregnancy (we offer prenatal adjustments instead)
- Severe osteoporosis (T-score below -2.5)
- An unstable spinal fracture or active spinal infection
- An abdominal aortic aneurysm
seek emergency care if you have:
- Bowel or bladder dysfunction (loss of control or inability to urinate)
- Saddle numbness (loss of sensation between your legs)
- Progressive weakness in both legs
- Severe pain following significant trauma
EVIDENCE-BASED OUTCOMES
What the Research Says About Spinal Decompression
Reported significant pain reduction
(Shealy & Borgmeyer, 1997)
Improvements maintained at follow-up
(Macario & Pergolizzi, 2006)
Negative intradiscal pressure achieved
(Moore et al., 2019)

Clinical Outcome Studies
In a study of 778 patients with herniated and degenerative discs, 86% reported immediate resolution or significant improvement. Decompression therapy appears particularly effective for patients who have failed other conservative treatments.
Mechanism of Action Research
Ramos & Martin demonstrated that controlled distraction forces produce measurable negative intradiscal pressure, dropping to -100 to -200 mmHg within the disc space—levels sufficient to promote disc retraction.
Disc Healing & Regeneration Evidence
Cyclic loading and unloading of intervertebral discs stimulates disc cell metabolism and promotes proteoglycan synthesis. This creates conditions for actual disc tissue repair rather than just temporary symptom relief.
Our Integrated Approach to Spinal Decompression

Comprehensive Assessment
Visit 1 includes a 3D biomechanical examination and full-spine digital X-rays to evaluate alignment, joint mobility, and structural integrity before any treatment begins.
Report of Findings
Visit 2 reviews all imaging. If decompression is appropriate, you receive a detailed care plan specifying the number of sessions (typically 12 or 24) and expected milestones.
The DOC Protocol
We precisely program the table's distraction angle, patient positioning, and force parameters based on the specific target disc level and your unique pathology.
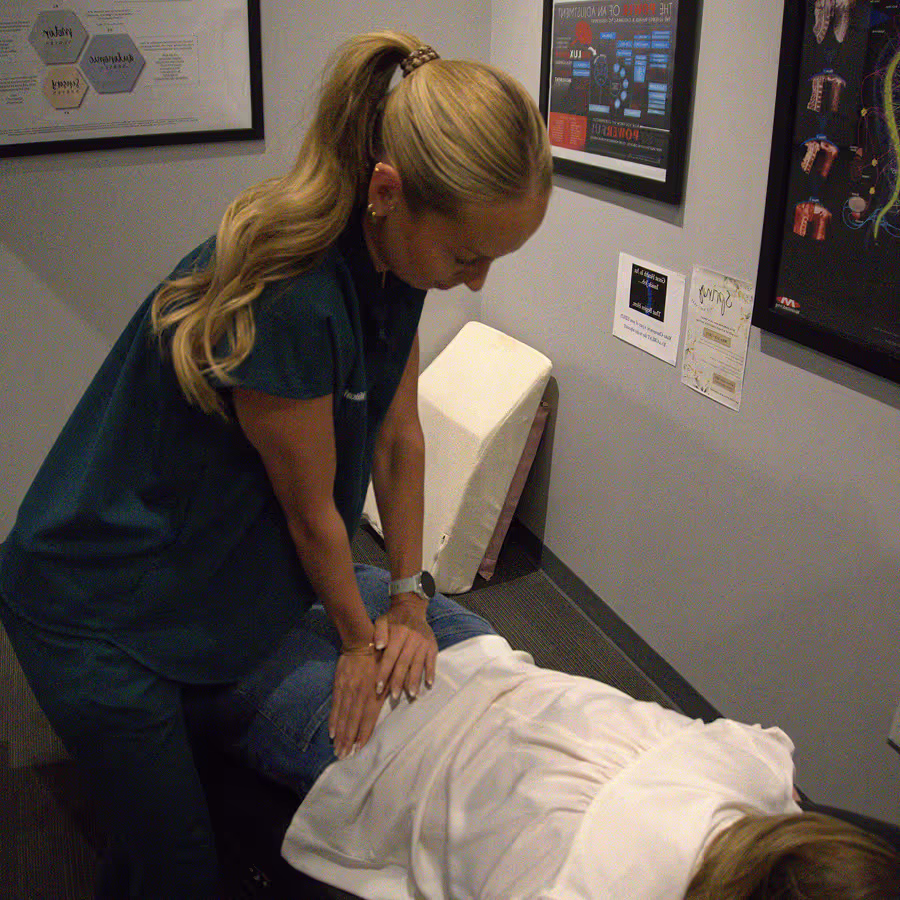
Integrated Corrective Care
We combine decompression with structural chiropractic adjustments to fix misalignment, Pettibon corrective protocols for posture, and access to our recovery suite.
What to Expect During Your Treatment: The Decompression Process
STEP 01
Before the Session
Most patients begin with 3 sessions per week. Wear loose-fitting clothing and avoid large meals beforehand to ensure maximum comfort on the table.
STEP 02
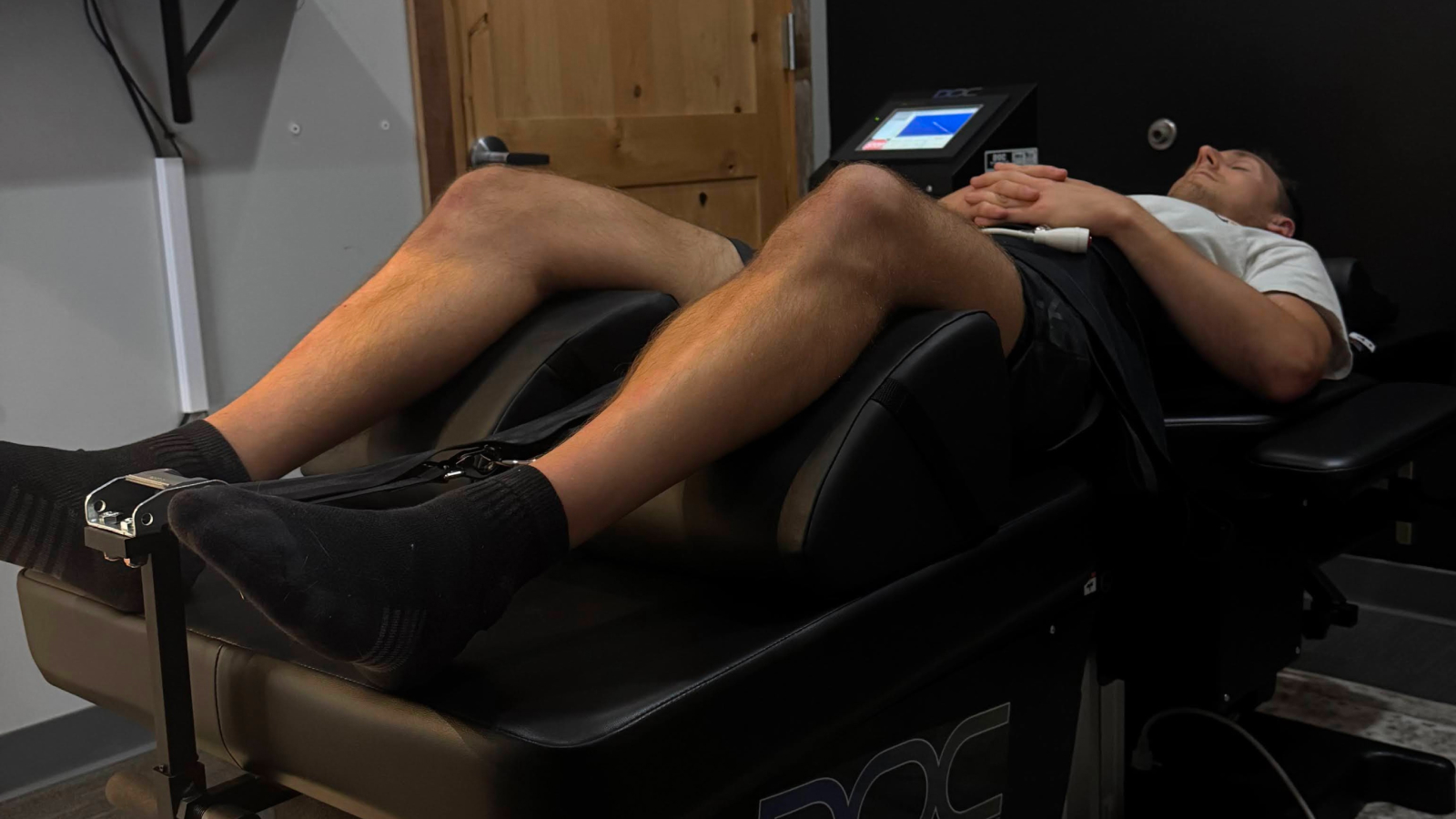
During Decompression
Secured in the DOC table, you'll feel a gentle, comfortable cyclic stretching (15-25 minutes). Many patients find it so relaxing they fall asleep.
STEP 03
After the Session
Dr. Booher may perform complementary adjustments. You can utilize our recovery room (infrared sauna/cold plunge) to reduce inflammation.
Progress Milestones to Monitor
Initial Relief (Sessions 1-8)
- Sessions 1-4: Temporary relief during and immediately after sessions. Symptoms may return between visits (this is normal). Minor soreness may occur.
- Sessions 5-8: Relief begins lasting longer between sessions. Many patients report reduced radiating leg or arm pain and improved mobility.
Sustained Improvement (Sessions 9-24)
- Sessions 9-12: Significant symptom improvement. Functional activities that were previously painful become manageable. Reassessment occurs here.
- Sessions 13-24: Progressive structural improvement for more severe cases. Disc hydration and healing continue, and symptoms stabilize.
CLINICAL HONESTY
When Decompression May Not Be the Right Fit
While decompression demonstrates strong clinical evidence, it is not appropriate for every patient. If you have spinal fusion hardware (rods, screws, cages), are pregnant, have severe osteoporosis, or have unstable spinal fractures, decompression therapy is contraindicated. We evaluate surgical history (like simple discectomies) on a case-by-case basis.
If your pain is primarily from facet joints rather than disc pathology, standard chiropractic adjustments may be more appropriate and cost-effective. We maintain referral relationships with orthopedic spine surgeons and pain management physicians to ensure coordinated care if you have progressive neurological deficits or require combined approaches like epidural injections.
Common Questions About Spinal Decompression
Standard mechanical traction applies a constant pulling force, which triggers the body’s protective muscle guarding reflex—your muscles tighten to resist the pull. True spinal decompression uses computerized variable force curves that gradually cycle between pulling and releasing in patterns the body cannot anticipate. This achieves genuine negative intradiscal pressure that traction simply cannot replicate.
The number of sessions is determined by your examination findings—it’s not a one-size-fits-all protocol. Dr. Mikala Booher typically recommends either 12 or 24 sessions based on condition severity. Research shows most patients experience meaningful improvement within the first 4–6 sessions, with optimal outcomes achieved through completion of the full protocol.
An MRI is helpful but not required to begin. Dr. Booher takes full-spine digital X-rays during your initial visit, which reveal disc height loss and structural changes. If you have existing MRI results, bring them to help refine your protocol. In some cases, we may recommend obtaining an MRI if findings suggest it would meaningfully change the treatment approach.
Most patients find decompression therapy comfortable—many actually fall asleep during sessions. You’ll feel a gentle, cyclic stretching sensation. There should be no sharp or shooting pain. Some patients experience mild soreness for 24–48 hours after the first few sessions as tissues adapt. If you experience discomfort, parameters are adjusted immediately.
Elite Wellness Chiropractic is a cash-pay practice. Most insurance plans do not cover spinal decompression therapy, classifying it as investigational despite growing evidence. We do accept HSA and FSA payments. Your $60 New Patient Experience covers the comprehensive exam and X-rays, and Dr. Booher presents full treatment costs upfront.
It depends. If your surgery involved hardware placement (spinal fusion with rods, screws, or cages), decompression is contraindicated in that area to protect the implant. However, if you had a simple discectomy or laminectomy without hardware, decompression may still be appropriate. We evaluate surgical history on a case-by-case basis.
Decompression directly creates negative pressure to retract herniated material and promote healing. Chiropractic adjustments restore proper vertebral alignment, reducing the mechanical stresses that contributed to the disc damage initially. This integrated approach addresses the full biomechanical picture rather than treating a single component in isolation.
Still have questions?
What Our Patients Say About Disc Pain Relief
Celia L.
Bee Cave, TX
"For the last three weeks I've visited Dr. Mikala... I thoroughly enjoy their unique approach to treating the whole body. I work in the dental field, yrs of leaning awkwardly have reeked havoc. With Dr. Mikala's help the discomfort my sciatic nerve produced is almost nonexistent. The office staff is so welcoming!"
Robert T.
Lakeway, TX
"I was told surgery was my only option for my L4-L5 herniation. I could barely walk to my mailbox. Dr. Booher put me on a decompression and adjustment protocol. Three months later, I am fully avoiding the operating room and playing golf again."
Amanda W.
Westlake, TX
"The shooting pain down my leg was unbearable. The Elite Wellness team didn't just 'crack my back'—they mapped exactly which nerve was compressed and systematically took the pressure off. Truly life-changing non-surgical care."
Related Conditions We Also Treat
Bee Cave's Only DOC Decompression Table - Start Your Recovery Today
If you haven't found lasting relief from medication, injections, or physical therapy alone, spinal decompression therapy may be the missing piece. We combine true spinal decompression with structural corrective care to address the root cause of your disc-related pain.
*Dr. Mikala Booher, DC serves Bee Cave, Lakeway, West Lake Hills, Dripping Springs, and Southwest Austin.
Adams, M. A., & Roughley, P. J. (2006). What is intervertebral disc degeneration, and what causes it? Spine, 31(18), 2151-2161.
Apfel, C. C., Cakmakkaya, O. S., Martin, W., et al. (2010). Restoration of disk height through non-surgical spinal decompression is associated with decreased discogenic low back pain: a retrospective cohort study. BMC Musculoskeletal Disorders, 11, 155.
Arun, R., Freeman, B. J., Scammell, B. E., et al. (2009). 2009 ISSLS Prize Winner: What influence does sustained mechanical load have on diffusion in and degeneration of the intervertebral disc? An in vivo study using serial postcontrast magnetic resonance imaging. Spine, 34(21), 2324-2337.
Gionis, T. A., & Groteke, E. (2003). Spinal decompression. Orthopedic Technology Review, 5(6), 36-39.
Gose, E. E., Naguszewski, W. K., & Naguszewski, R. K. (1998). Vertebral axial decompression therapy for pain associated with herniated or degenerated discs or facet syndrome: an outcome study. Neurological Research, 20(3), 186-190.
Guehring, T., Omlor, G. W., Lorenz, H., et al. (2006). Disc distraction shows evidence of regenerative potential in degenerated intervertebral discs as evaluated by protein expression, magnetic resonance imaging, and messenger ribonucleic acid expression analysis. Spine, 31(15), 1658-1665.
Macario, A., & Pergolizzi, J. V. (2006). Systematic literature review of spinal decompression via motorized traction for chronic discogenic low back pain. Pain Practice, 6(3), 171-178.
Ozturk, B., Gunduz, O. H., Ozoran, K., & Bostanoglu, S. (2006). Effect of continuous lumbar traction on the size of lumbar disc herniation. Rheumatology International, 26(7), 622-626.
Ramos, G., & Martin, W. (1994). Effects of vertebral axial decompression on intradiscal pressure. Journal of Neurosurgery, 81(3), 350-353.
Shealy, C. N., & Borgmeyer, V. (1997). Decompression, reduction, and stabilization of the lumbar spine: a cost-effective treatment for lumbosacral pain. American Journal of Pain Management, 7, 63-65.