320+ 5-Star Google Reviews
Google Reviews
Non-Surgical Care for Disc Herniations & Bulges
Suffering from debilitating pain caused by disc issues? At Elite Wellness Chiropractic in Bee Cave, we specialize in identifying and correcting the underlying spinal dysfunction that contributes to disc herniations and bulges, empowering you to reclaim comfort and function without surgery.
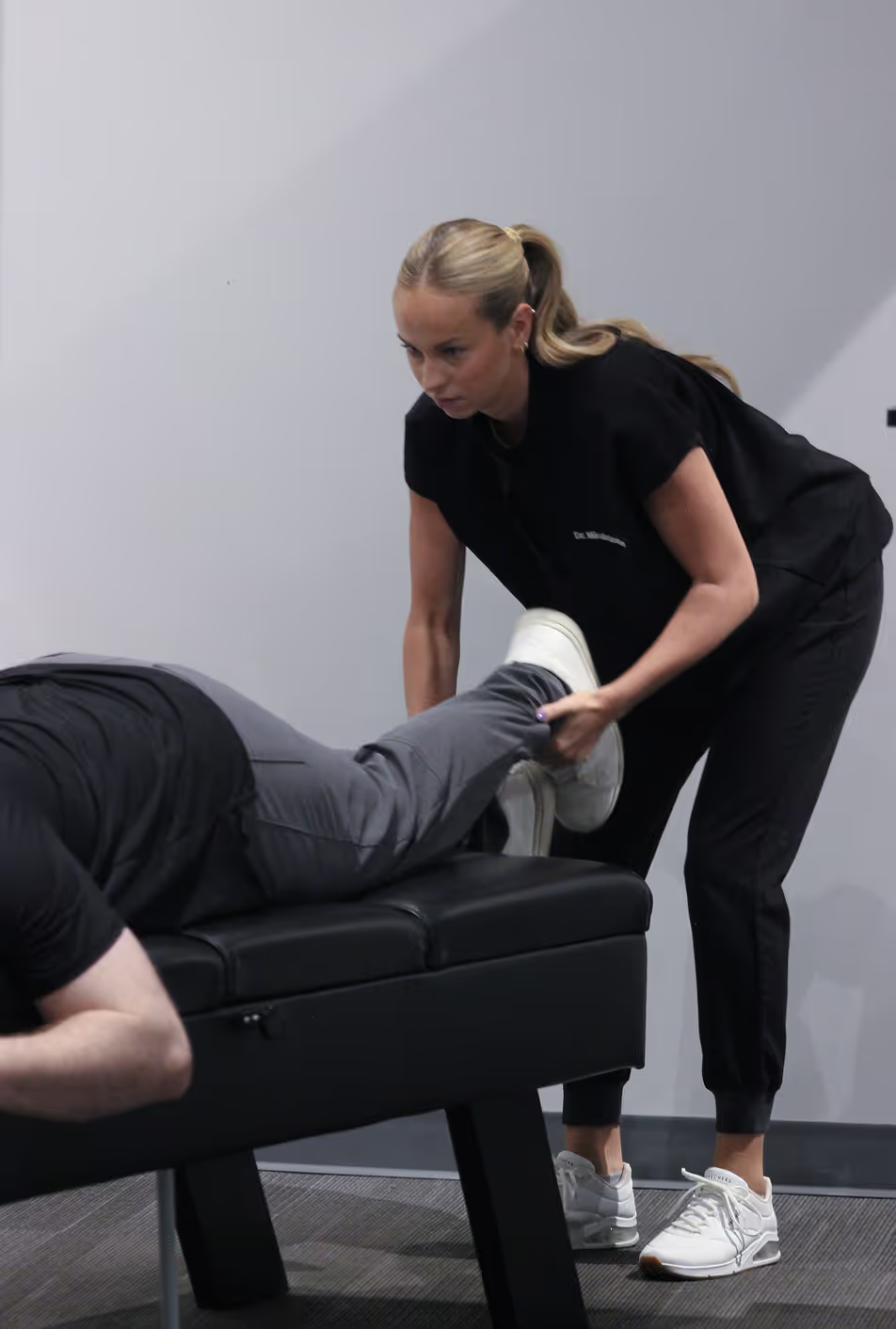
Key Takeaways: What You Need To Know About Disc Herniation Treatment
- Conservative care works: McMorland et al. (2010) found that 60% of herniated disc patients avoided surgery with spinal manipulation therapy compared to only 20% in surgical consultation groups.
- Early intervention matters: If you experience radiating leg pain, numbness, or weakness lasting more than 2 weeks, evidence shows prompt chiropractic treatment can prevent progression.
- Natural healing timeline: Peul et al. (2007) demonstrated that 75% of disc herniation patients achieve significant improvement within 12 weeks of conservative care.
- Multimodal approach superiority: Bronfort et al. (2004) showed that combining spinal adjustments with targeted exercises produces 40% better outcomes on disability scores.
- Safety profile: Thiel et al. (2007) found serious adverse events occur in less than 0.001% of chiropractic treatments, making it safer than most prescription medications for disc conditions.
- Emergency warning: If you develop bowel or bladder dysfunction, saddle numbness, or progressive weakness in both legs, this indicates cauda equina syndrome requiring immediate care.
Understanding Disc Herniations & Bulges - What's Actually Happening
Your intervertebral discs serve as sophisticated shock absorbers between each vertebra. When these structures fail, two distinct problems can occur: a disc bulge (where outer fibers weaken) or a true herniation (where inner gel breaks through).

The "Double-Crush" Mechanism
The pain you experience isn't just from mechanical compression. Kuslich et al. (1991) discovered that only 65% of sciatica symptoms result from direct nerve compression - the rest comes from chemical inflammation irritating the nerve roots.
The Inflammatory Cascade
Leaked disc material contains phospholipase A2, a key inflammatory mediator. This explains why some patients experience severe pain even with relatively small herniations. The inflammation can actually reduce local nerve conduction velocity.
Why Spinal Mechanics Matter
This deep understanding explains why our approach focuses not just on mechanical correction, but also on reducing inflammatory pressure and restoring normal nerve function through precise, evidence-based realignment.
Signs, Symptoms & When to Pay Attention
Lumbar Disc Symptoms
- Sharp, stabbing pain in the lower back
- Sciatica: pain radiating to the buttock, calf, or foot
- Numbness/tingling in legs or feet
- Pain worsens with sitting, bending, and coughing
Cervical Disc Symptoms
- Neck pain with radiation down the arm
- Shoulder blade pain and muscle spasms
- Numbness or tingling in the hands
- Grip strength weakness
Clinical Assessment
- Positive straight leg raise test
- Specific myotomal/dermatomal mapping
- 91% sensitivity for clinical detection when properly assessed
SEEK IMMEDIATE EMERGENCY CARE IF:
- Bowel or bladder dysfunction (inability to urinate, incontinence)
- Saddle anesthesia (numbness in the genital/anal region)
- Progressive weakness in both legs
- Severe pain accompanied by a fever
- Pain following significant trauma with neurological symptoms
Contact Us Within 24 Hours If
- You experience new onset of foot drop or severe muscle weakness
- Numbness or tingling is rapidly worsening
- Pain consistently awakens you from sleep
- Symptoms haven't improved after 2 weeks of prior conservative care
EVIDENCE-BASED OUTCOMES
What the Research Says About Chiropractic Care for Disc Herniations
Avoided surgery completely
(McMorland et al., 2010)
Significantly improved within 12 weeks
(Peul et al., 2007)
Better outcomes with multimodal care
(Bronfort et al., 2004)

Breakthrough Research on Surgery Avoidance
McMorland et al. (2010) found that 60% of patients successfully avoided surgery with spinal manipulation compared to only 20% in the surgical consultation group. This represents a threefold improvement in surgical avoidance rates.
Systematic Review Evidence
The Cochrane Collaboration published findings analyzing 26 RCTs involving 6,070 patients. They found moderate evidence that spinal manipulation provides statistically significant improvements in both pain and function for chronic low back pain, including disc conditions.
Comparative Effectiveness
The SPORT trial followed 501 patients for 4 years. While surgical patients improved faster initially, both groups had similar long-term outcomes, proving conservative care achieves equivalent results without the surgical risks.
Expert Herniated Disc Treatment: Our Approach

Comprehensive Assessment
Detailed neurological and orthopedic testing including Lasegue's sign and precise dermatomal mapping to identify the exact level of disc involvement (85% diagnostic accuracy).
Precision Adjustments
Utilizing specific high-velocity, low-amplitude manual techniques or the gentler instrument-assisted Activator Method based on your acute pain levels and presentation.
Spinal Decompression
Integrating non-surgical decompression therapy, proven to reduce VAS pain scores and significantly improve Oswestry Disability Index scores by relieving direct pressure.
Rigorous Reassessment
Following evidence-based protocols, we reassess patients every 2 weeks during the initial phase. Failure to show improvement by 4 weeks warrants immediate treatment modification.
Your Clear Path to Disc Pain Relief:
Our Non-Surgical 3-Step Process
STEP 01
Comprehensive Discovery
Comprehensive biomechanical exam + digital X-rays (if needed). Dr. Booher identifies the exact structural causes of your pain.
STEP 02
Personalized Corrective Plan
We design a tailored non-surgical plan of precise adjustments, decompression, and targeted therapies for lasting relief.
STEP 03
Achieve & Maintain Results
Through consistent care, you'll find relief, facilitate natural disc healing, and build resilience for long-term spinal health.
What to Expect During Treatment
1 Initial & Active Phases (Weeks 1-8)
- Weeks 1-2:Gentle techniques to reduce acute inflammation. Specific ice/heat protocols. Expected 20-30% reduction in daily pain.
- Weeks 3-8:Advancing to targeted adjustments and exercise programming. Frequency at 2-3 times/week.
- Milestone (Week 6): Return to most normal activities without significant pain increase for the majority of patients.
Stabilization Phase (Weeks 9-12)
- Focus: Maintenance and prevention focus (1-2 times/week). Emphasizing postural correction and ergonomic education.
- Home Care: Specific self-assessment techniques, pain tracking, and advanced strengthening to prevent recurrence.
- Milestone (Week 12): Achievement of long-term stability. Research shows 90% of substantial improvement occurs within this window.
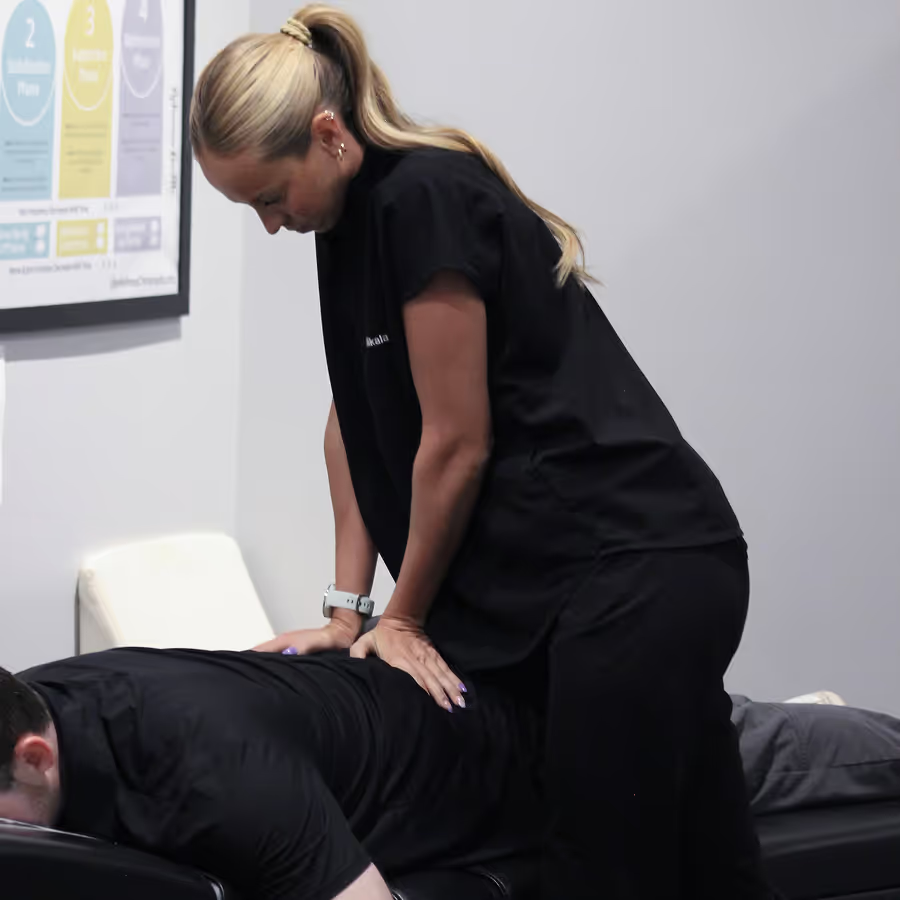
CLINICAL HONESTY
When Chiropractic Care May Not Be the Right Fit
Transparency builds trust and ensures your safety. While chiropractic care demonstrates excellent outcomes for most disc cases, absolute contraindications include Cauda Equina Syndrome (a surgical emergency), rapidly progressive neurological deficits, severe central stenosis with myelopathy, and active malignancies. We rigorously screen for these red flags at your first visit.
For patients with acute disc sequestration (free fragments), severe inflammatory conditions, or those on heavy anticoagulant therapy, we modify our approach or co-manage with specialists. If conservative measures do not yield measurable improvement, we actively coordinate with pain management doctors, neurologists, or orthopedic surgeons to ensure you get the right care.
Common Questions About Disc Herniations & Bulges
Disc-related pain typically creates specific patterns that differ from muscle strain. Kuslich et al. (1991) found that disc herniations produce radiating pain into the leg (sciatica), numbness following specific nerve distributions, and pain that worsens with sitting, bending forward, or coughing. Muscle strains usually cause localized pain that improves with movement.
Yes, chiropractic care has an excellent safety profile for disc conditions when properly applied. Thiel et al. (2007) studied 19,722 patients and found no serious adverse events. Dr. Mikala Booher performs comprehensive screening to identify rare contraindications like cauda equina syndrome. The key is proper patient selection and technique modification.
Peul et al. (2007) found that 75% of patients achieve significant improvement within 12 weeks of conservative care, with most progress occurring in the first 6 weeks. Santilli et al. (2006) showed that improvements typically begin within the first 2 weeks. We reassess progress every 2 weeks and expect measurable improvement by the 4-week mark.
While adjustments don’t “push the disc back in,” they create optimal conditions for natural healing. Spinal manipulation restores proper alignment, reduces pressure, and improves blood flow. This anti-inflammatory effect reduces the chemical irritation identified by McCarron et al. Many disc herniations reabsorb naturally over time while we manage your symptoms.
Avoid prolonged sitting, heavy lifting with improper mechanics, repetitive bending and twisting, and high-impact activities during acute phases. Forward bending exercises like toe touches increase disc pressure and should be avoided. However, gentle walking and specific exercises prescribed by Dr. Booher can accelerate your recovery.
While 60% avoid surgery with conservative care (McMorland et al.), surgery is required for cauda equina syndrome, progressive muscle weakness unresponsive to conservative care within 6–8 weeks, or massive disc herniations causing severe neurological compromise. Note that the SPORT trial showed surgery and conservative care achieve similar long-term outcomes at 4 years.
X-rays help evaluate spinal alignment but don’t show discs directly. MRI provides detailed visualization but isn’t always necessary initially. Guidelines recommend against routine lumbar MRI in the first 6 weeks unless red flags are present. Dr. Booher uses clinical examination findings to guide imaging decisions when symptoms don’t improve as expected.
Still have questions?
What Our Patients Say About Disc Pain Relief
Celia Leung
Bee Cave, TX
"For the last three weeks I've visited Dr. Mikala... I thoroughly enjoy their unique approach to treating the whole body. I work in the dental field, yrs of leaning awkwardly have reeked havoc. With Dr. Mikala's help the discomfort my sciatic nerve produced is almost nonexistent. The office staff is so welcoming!"
Celia Leung
Lakeway, TX
"I was told surgery was my only option for my L4-L5 herniation. I could barely walk to my mailbox. Dr. Booher put me on a decompression and adjustment protocol. Three months later, I am fully avoiding the operating room and playing golf again."
Amanda W.
Westlake, TX
"The shooting pain down my leg was unbearable. The Elite Wellness team didn't just 'crack my back'—they mapped exactly which nerve was compressed and systematically took the pressure off. Truly life-changing non-surgical care."
Related Conditions We Also Treat
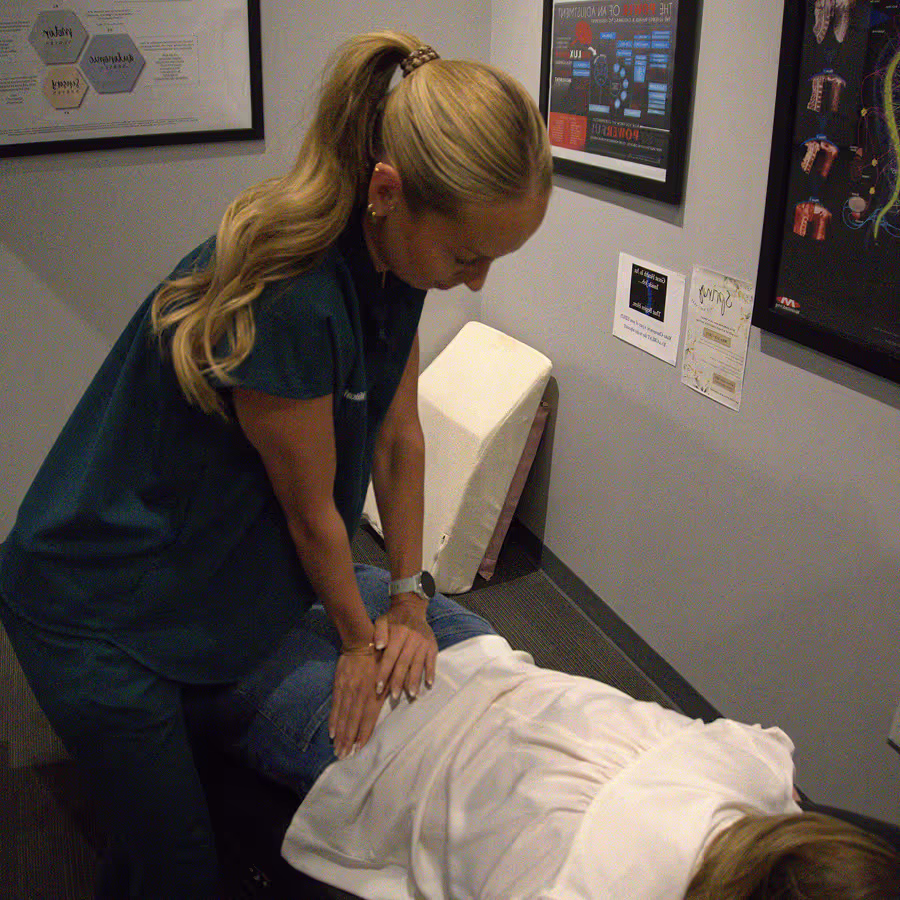
Start Your Recovery Journey with Our Bee Cave Team
Don't let lower back pain control your life any longer. Research consistently demonstrates that early intervention produces the best outcomes. The longer you wait, the more likely your acute pain becomes chronic.
*Dr. Mikala Booher, DC serves Bee Cave, Lakeway, West Lake Hills, Dripping Springs, and Southwest Austin.
Atlas, S. J., Keller, R. B., Wu, Y. A., Deyo, R. A., & Singer, D. E. (2005). Long-term outcomes of surgical and nonsurgical management of sciatica secondary to a lumbar disc herniation: 10 year results from the maine lumbar spine study. Spine, 30(8), 927-935.
Apfel, C. C., Cakmakkaya, O. S., Martin, W., Richmond, C., Macario, A., George, E., ... & Pergolizzi, J. V. (2010). Restoration of disk height through non-surgical spinal decompression is associated with decreased discogenic low back pain: a retrospective cohort study. BMC Musculoskeletal Disorders, 11, 155.
Ahn, U. M., Ahn, N. U., Buchowski, J. M., Garrett, E. S., Sieber, A. N., & Kostuik, J. P. (2000). Cauda equina syndrome secondary to lumbar disc herniation: a meta-analysis of surgical outcomes. Spine, 25(12), 1515-1522.
Bronfort, G., Haas, M., Evans, R. L., & Bouter, L. M. (2004). Efficacy of spinal manipulation and mobilization for low back pain and neck pain: a systematic review and best evidence synthesis. The Spine Journal, 4(3), 335-356.
Cassidy, J. D., Boyle, E., Côté, P., He, Y., Hogg-Johnson, S., Silver, F. L., & Bondy, S. J. (2008). Risk of vertebrobasilar stroke and chiropractic care: results of a population-based case-control and case-crossover study. Spine, 33(4S), S176-S183.
Cherkin, D. C., Deyo, R. A., Battié, M., Street, J., & Barlow, W. (1998). A comparison of physical therapy, chiropractic manipulation, and provision of an educational booklet for the treatment of patients with low back pain. New England Journal of Medicine, 339(15), 1021-1029.
Chou, R., Qaseem, A., Snow, V., Casey, D., Cross Jr, J. T., Shekelle, P., ... & Owens, D. K. (2007). Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society. Annals of Internal Medicine, 147(7), 478-491.
Copay, A. G., Glassman, S. D., Subach, B. R., Berven, S., Schuler, T. C., & Carreon, L. Y. (2008). Minimum clinically important difference in lumbar spine surgery patients: a choice of methods using the Oswestry Disability Index, Medical Outcomes Study questionnaire Short Form 36, and pain scales. The Spine Journal, 8(6), 968-974.
Deville, W. L., van der Windt, D. A., Dzaferagic, A., Bezemer, P. D., & Bouter, L. M. (2000). The test of Lasègue: systematic review of the accuracy in diagnosing herniated discs. Spine, 25(9), 1140-1147.
Ernst, E. (2002). A systematic review of systematic reviews of spinal manipulation. Journal of the Royal Society of Medicine, 95(2), 55-62.
Fritz, J. M., Cleland, J. A., & Childs, J. D. (2007). Subgrouping patients with low back pain: evolution of a classification approach to physical therapy. Journal of Orthopaedic & Sports Physical Therapy, 37(6), 290-302.
Hestbaek, L., Leboeuf-Yde, C., & Manniche, C. (2003). Low back pain: what is the long-term course? A review of studies of general patient populations. European Spine Journal, 12(2), 149-165.
Hurwitz, E. L., Morgenstern, H., Harber, P., Kominski, G. F., Yu, F., & Adams, A. H. (2002). A randomized trial of chiropractic manipulation and mobilization for patients with neck pain: clinical outcomes from the UCLA neck-pain study. American Journal of Public Health, 92(10), 1634-1641.
Jarvik, J. G., & Deyo, R. A. (2002). Diagnostic evaluation of low back pain with emphasis on imaging. Annals of Internal Medicine, 137(7), 586-597.
Jordan, K., Dunn, K. M., Lewis, M., & Croft, P. (2006). A minimal clinically important difference was derived for the Roland-Morris Disability Questionnaire for low back pain. Journal of Clinical Epidemiology, 59(1), 45-52.
Kobayashi, S., Yoshizawa, H., & Nakai, S. (2005). Experimental study on the dynamics of lumbosacral nerve root circulation. Spine, 30(8), 919-923.
Kuslich, S. D., Ulstrom, C. L., & Michael, C. J. (1991). The tissue origin of low back pain and sciatica: a report of pain response to tissue stimulation during operations on the lumbar spine using local anesthesia. Orthopedic Clinics of North America, 22(2), 181-187.
Lewis, R. A., Williams, N. H., Sutton, A. J., Burton, K., Din, N. U., Hendry, M., ... & Wilkinson, C. (2015). Comparative clinical effectiveness of management strategies for sciatica: systematic review and network meta-analyses. The Spine Journal, 15(6), 1461-1477.
McCarron, R. F., Wimpee, M. W., Hudkins, P. G., & Laros, G. S. (1987). The inflammatory effect of nucleus pulposus. A possible element in the pathogenesis of low-back pain. Spine, 12(8), 760-764.
McMorland, G., Suter, E., Casha, S., du Plessis, S. J., & Hurlbert, R. J. (2010). Manipulation or microdiskectomy for sciatica? A prospective randomized clinical study. Journal of Manipulative and Physiological Therapeutics, 33(8), 576-584.
Olmarker, K., & Rydevik, B. (1991). Pathophysiology of sciatica. Orthopedic Clinics of North America, 22(2), 223-234.
Ostelo, R. W., Deyo, R. A., Stratford, P., Waddell, G., Croft, P., Von Korff, M., ... & de Vet, H. C. (2008). Interpreting change scores for pain and functional status in low back pain: towards international consensus regarding minimal important change. Spine, 33(1), 90-94.
Paige, N. M., Miake-Lye, I. M., Booth, M. S., Beroes, J. M., Mardian, A. S., Dougherty, P., ... & Shekelle, P. G. (2017). Association of spinal manipulative therapy with clinical benefit and harm for acute low back pain: systematic review and meta-analysis. JAMA, 317(14), 1451-1460.
Peul, W. C., van Houwelingen, H. C., van den Hout, W. B., Brand, R., Eekhof, J. A., Tans, J. T., ... & Koes, B. W. (2007). Surgery versus prolonged conservative treatment for sciatica. New England Journal of Medicine, 356(22), 2245-2256.
Rubinstein, S. M., Terwee, C. B., Assendelft, W. J., de Boer, M. R., & van Tulder, M. W. (2012). Spinal manipulative therapy for chronic low-back pain. Cochrane Database of Systematic Reviews, (9).
Santilli, V., Beghi, E., & Finucci, S. (2006). Chiropractic manipulation in the treatment of acute back pain and sciatica with disc protrusion: a randomized double-blind clinical trial of active and simulated spinal manipulations. The Spine Journal, 6(2), 131-137.
Thiel, H. W., Bolton, J. E., Docherty, S., & Portlock, J. C. (2007). Safety of chiropractic manipulation of the cervical spine: a prospective national survey. Spine, 32(21), 2375-2378.
Vroomen, P. C., de Krom, M. C., Wilmink, J. T., Kester, A. D., & Knottnerus, J. A. (2002). Diagnostic value of history and physical examination in patients suspected of lumbosacral nerve root compression. Journal of Neurology, Neurosurgery & Psychiatry, 72(5), 630-634.
Weber, H. (1983). Lumbar disc herniation: a controlled, prospective study with ten years of observation. Spine, 8(2), 131-140.
Weinstein, J. N., Tosteson, T. D., Lurie, J. D., Tosteson, A. N., Hanscom, B., Skinner, J. S., ... & Herkowitz, H. (2006). Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT): a randomized trial. JAMA, 296(20), 2441-2450.