320+ 5-Star Google Reviews
Google Reviews
Expert Sciatica Treatment in Bee Cave, TX
Tired of radiating pain, numbness, or tingling down your leg? At Elite Wellness Chiropractic, we specialize in identifying and correcting the spinal and nerve issues that cause sciatica, empowering you to reclaim comfort and mobility.
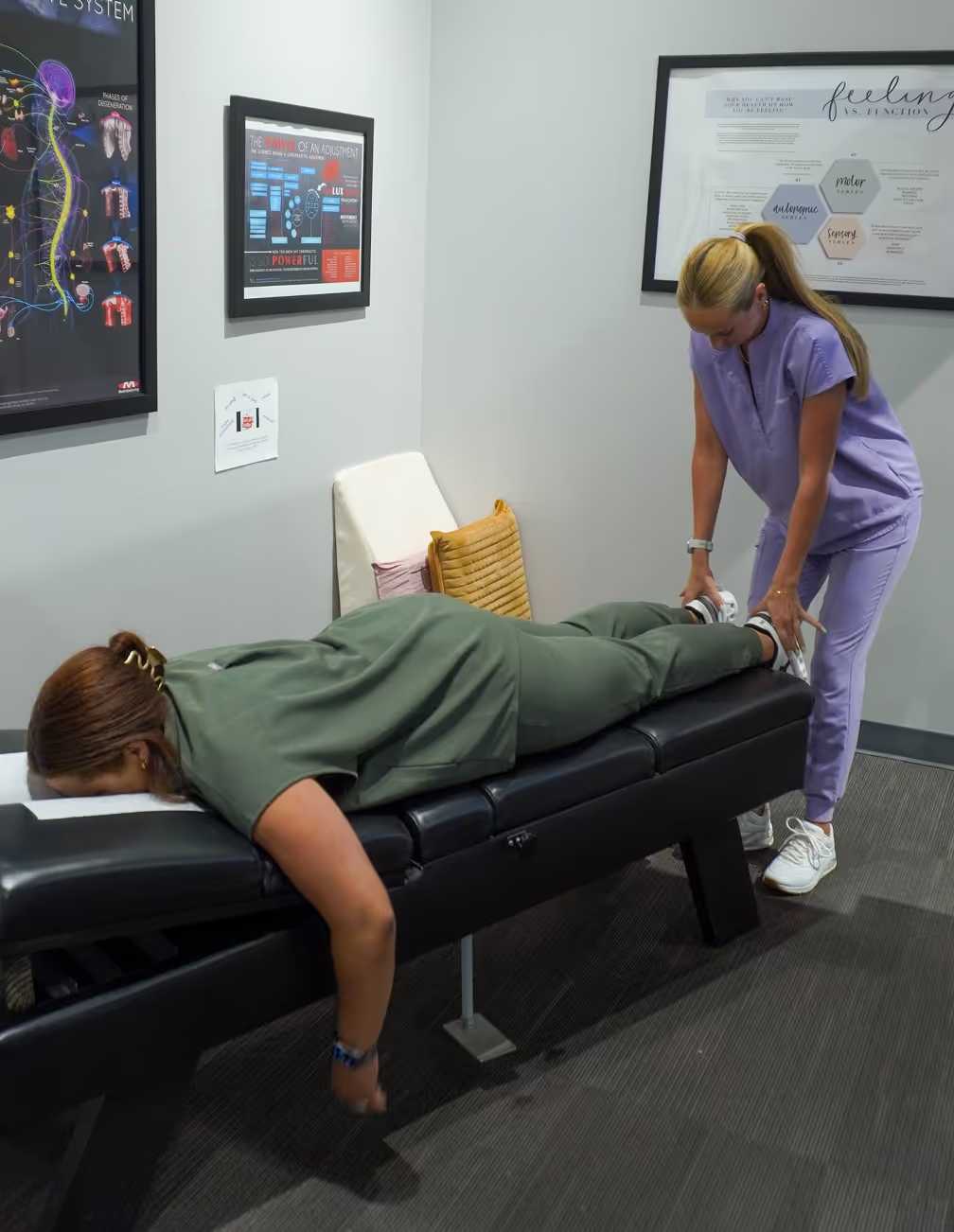
Key Takeaways: What You Need To Know About Sciatica Treatment
- Sciatica affects the sciatic nerve pathway from L4-S3 nerve roots, with 85-90% of cases caused by lumbar disc herniation creating both mechanical compression and inflammatory responses (Lewis et al., 2007)
- Chiropractic manipulation shows 60% success rates compared to 40% for surgery in treating acute sciatica, with mean Oswestry Disability Index improvements of 25.1 points versus 16.5 points for surgical intervention (McMorland et al., 2010)
- 90% of sciatica patients experience resolution within 12 weeks of conservative treatment (Pengel et al., 2003), with reassessment every 2 weeks to track progress and adjust protocols
- 50% improvement in pain scores typically occurs by week 4 of chiropractic treatment, with early improvement at 2 weeks being a strong predictor of success (Fritz et al., 2005)
- If symptoms persist beyond 6 weeks without improvement, MRI evaluation and specialist consultation should be considered to rule out surgical indications
- Emergency Warning: If sciatica symptoms include bowel/bladder dysfunction, saddle anesthesia, or bilateral leg weakness, seek emergency medical attention immediately (potential cauda equina syndrome)
Understanding Sciatica - What's Actually Happening in Your Body
Sciatica represents irritation or compression of the sciatic nerve, which originates from nerve roots L4 through S3 in your lumbar spine and extends through your hip, buttock, and down each leg. The sciatic nerve is the largest nerve in your body.

Mechanical Compression & Inflammation
The pathophysiology involves two critical components. Takahashi et al. (2003) demonstrated that mechanical compression alone is insufficient. Instead, nerve root inflammation creates the chemical irritation that generates your radiating pain, numbness, and weakness.
The Role of Disc Herniation
Lewis et al. (2007) identified that herniated nucleus pulposus - the inner gel-like material of spinal discs - creates direct pressure and triggers an inflammatory cascade. This explains why symptoms can vary so wildly between patients with similar structural changes.
Biomechanical Design
The lumbar spine's design contributes to sciatica development. Adams & Roughley (2006) found that disc degeneration patterns predispose to posterolateral herniation, with L4-L5 and L5-S1 levels most commonly affected due to increased mechanical stress.
Signs, Symptoms & When to Pay Attention
Primary Symptoms
- Sharp, shooting, or burning pain radiating down the leg
- Numbness/tingling (pins-and-needles)
- Weakness in the affected leg/foot
- Worsens with prolonged sitting, coughing, or sneezing
Secondary Symptoms
- Deep aching in the buttock region
- Muscle spasms in the lower back/hip
- Difficulty bearing weight on the affected leg
- Pain relief when walking or changing positions frequently
Assessment & Testing
- Unilateral leg pain greater than back pain
- Positive Straight Leg Raise (91% sensitivity)
- Positive Crossed Straight Leg Raise (88% specificity)
- Neurological deficits in L4-S3
Seek Immediate Emergency Care If
- Bowel or bladder dysfunction or incontinence
- Saddle anesthesia (numbness around the genital/anal region)
- Bilateral leg weakness affecting both legs
- Progressive motor weakness developing over hours
- Fever accompanying back and leg pain
Consider Chiropractic Evaluation If:
- Symptoms persist beyond 6 weeks without improvement
- Functional improvement plateaus despite pain reduction
- Occupational factors significantly contribute to symptom perpetuation
- You are considering invasive or surgical treatment options
EVIDENCE-BASED OUTCOMES
What the Research Says About Chiropractic Treatment for Sciatica
Success vs 40% for surgery
(McMorland et al., 2010)
Mean pain reduction (VAS scale)
(Coulter et al., 2018)
Of patients avoid surgery
(Peul et al., 2007)

Landmark Clinical Trials
McMorland et al. (2010) published a pivotal study comparing spinal manipulation to microdiscectomy in acute and subacute sciatica. Manipulation achieved 60% success rates compared to 40% for surgery at 2-year follow-up, with significantly greater functional improvements.
Systematic Evidence
Coulter et al. (2018) analyzed 12 randomized controlled trials involving 2,887 patients. Their meta-analysis revealed significant pain reduction and functional improvement with manual therapy approaches for sciatica.
Comparative Effectiveness
Peul et al. (2007) conducted the SPORT trial comparing early surgery to conservative care. While surgery provided faster initial relief, no differences existed between groups at 1-2 year follow-up, and 90% of conservative patients successfully avoided surgery.
Our Approach to Sciatica Treatment Bee Cave Patients Trust

Diagnostic Assessment
Thorough neurological and orthopedic examination including SLR and slump testing (84% sensitivity for identifying neural tension) to identify specific nerve involvement patterns.
Specialized Techniques
Manual chiropractic adjustments targeting lumbar spine dysfunction and pelvic adjustments addressing sacroiliac joint involvement. Decompressive techniques for disc-related sciatica cases.
Comprehensive Methodology
A structured Assessment → Treatment → Reassessment pathway. We integrate manual therapy with patient education and specific home care strategies.
Reassessment & Monitoring
Objective tracking using validated outcome measures every 2 weeks. Follow-up at 4-week intervals to monitor long-term stability and treatment progress.
Your Clear Path to Sciatica Relief:
Our 3-Step Process
STEP 01
Comprehensive Discovery
We conduct a thorough assessment, including X-rays if needed, to pinpoint the root cause of your sciatica.
STEP 02
Personalized Corrective Plan
We design a tailored treatment plan of precise adjustments and home care strategies for lasting relief.
STEP 03
Achieve & Maintain Results
Through consistent care, you'll find relief and build resilience for long-term well-being and mobility.
What to Expect During Treatment at Our Bee Cave Clinic
Initial & Active Phases (Weeks 1-6)
- Weeks 1-2 (Initial): Focus on reducing acute inflammation and nerve irritation. 2-3 visits/week. 25% improvement is typically seen.
- Weeks 3-6 (Active): Address underlying biomechanical dysfunction. 2 visits/week. Correcting spinal misalignments.
- Milestone: 50% improvement in functional measures typically occurs by week 4.
Stabilization Phase (Weeks 7-12)
- Focus: Maintain improvements, build spinal stability, and prevent recurrence. Transitioning to bi-weekly visits.
- Home Care: Specific positioning strategies, progressive stretching, and ergonomic education.
- Milestone: 90% resolution rates within 12 weeks of appropriate conservative management.
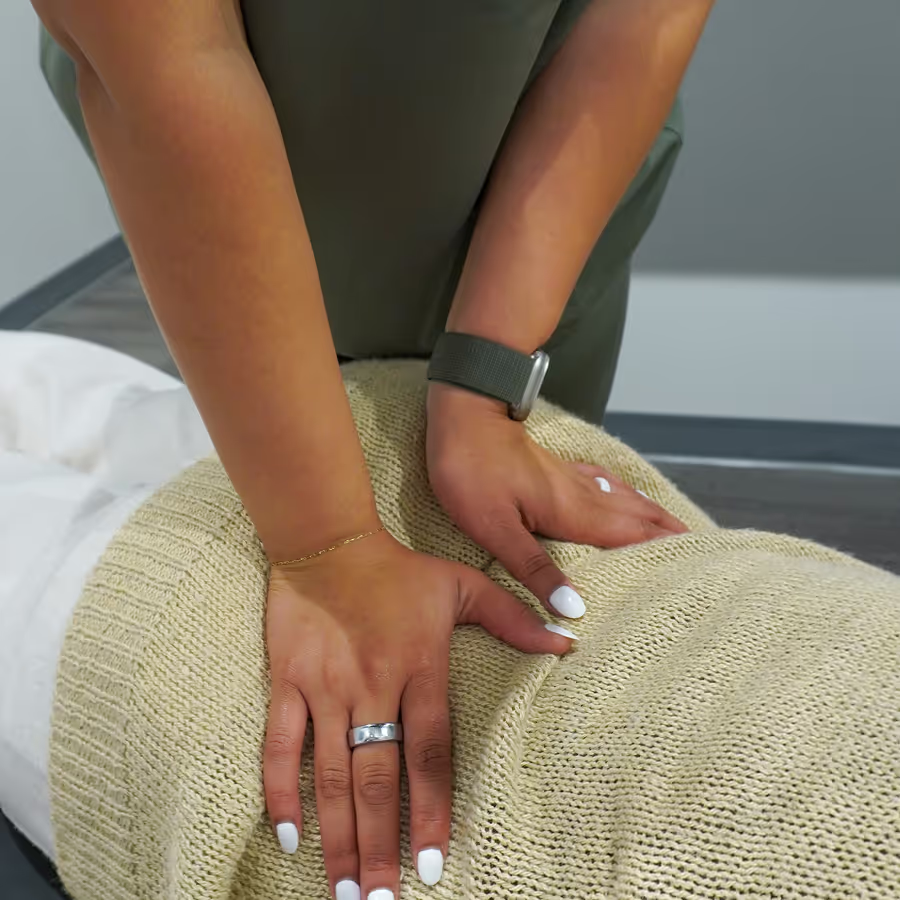
CLINICAL HONESTY
When Chiropractic Treatment May Not Be the Right Fit
While chiropractic care demonstrates excellent effectiveness for most sciatica cases, certain conditions require different approaches or immediate medical intervention. Dr. Booher performs a thorough screening to identify any absolute contraindications, such as cauda equina syndrome, severe progressive motor weakness, or malignancy, ensuring you are referred immediately if needed.
For patients on anticoagulation therapy or those with recent spinal surgery, we modify our approach using low-force techniques like the Activator method. If symptoms persist beyond 6-8 weeks without significant improvement, we readily coordinate advanced imaging, physical therapy, or specialist consultations.
Common Questions About Sciatica & Chiropractic Care
Sciatica typically presents as sharp, shooting, or burning pain that travels from your lower back through your buttock and down your leg, often extending below the knee. Seek immediate medical attention if you develop bowel or bladder dysfunction, saddle anesthesia around your genital area, or weakness in both legs — these symptoms indicate potential cauda equina syndrome requiring emergency intervention.
Research demonstrates excellent effectiveness. McMorland et al. (2010) found spinal manipulation achieved 60% success rates compared to 40% for surgery at 2-year follow-up. Coulter et al. (2018) meta-analysis showed significant pain reduction averaging 12.07 points on a Visual Analog Scale. 90% of patients avoid surgery when receiving appropriate conservative care.
Chiropractic manipulation maintains excellent safety profiles. Rubinstein et al. (2019) documented serious adverse events occurring in less than 1 in 10,000 treatments, while minor side effects like temporary soreness affect 50–60% of patients. Dr. Booher performs thorough neurological examination before treatment to identify any contraindications.
50% of patients experience significant relief within 6 weeks according to Delitto et al. (2012). Pengel et al. (2003) found 90% resolution rates within 12 weeks of appropriate treatment. Dr. Booher reassesses progress every 2 weeks, with most patients requiring 8–16 visits over 6–12 weeks depending on response.
Chou et al. (2011) guidelines recommend MRI only if symptoms persist beyond 6 weeks AND you’re considering surgery, or if red flag symptoms are present. Clinical examination, including straight leg raise testing (91% sensitivity), is highly effective for diagnosis. Digital X-rays may be utilized in-house to assess spinal alignment.
Your initial appointment includes comprehensive history taking, neurological examination, and orthopedic testing (slump tests, straight leg raises) to identify specific dysfunction patterns. X-rays may be taken if indicated. Treatment typically begins during the first visit with gentle manual adjustments. Expect the appointment to take 45–60 minutes.
Research strongly supports conservative care for avoiding surgical intervention. The SPORT trial (Peul et al., 2007) demonstrated that 90% of patients receiving conservative care successfully avoided surgery, with no long-term differences between surgical and conservative groups at 1–2 years. Our focus is providing natural alternatives for appropriate candidates.
Still have questions?
What Our Patients Say About Back Pain Relief
Larry Weisinger
Bee Cave, TX
"Elite Wellness is best Chiropractic Clinic in Central Texas. Dr. Mikala's expertise in spinal alignment is incredible. I came in with an old injury causing periodic sciatica pain. 3 weeks later, 90% reduction in these episodes!"
Elena R.
Lakeway, TX
"The shooting pain down my leg was so bad I couldn't sit for work. Dr. Booher identified the exact disc issue without rushing me to surgery. I'm finally pain-free and back to my normal life."
David K.
Westlake, TX
"They don't just 'crack' your back. It's a full corrective approach. My sciatica had been bothering me for months, but their specific adjustments and home stretches changed everything."
Related Conditions We Also Treat
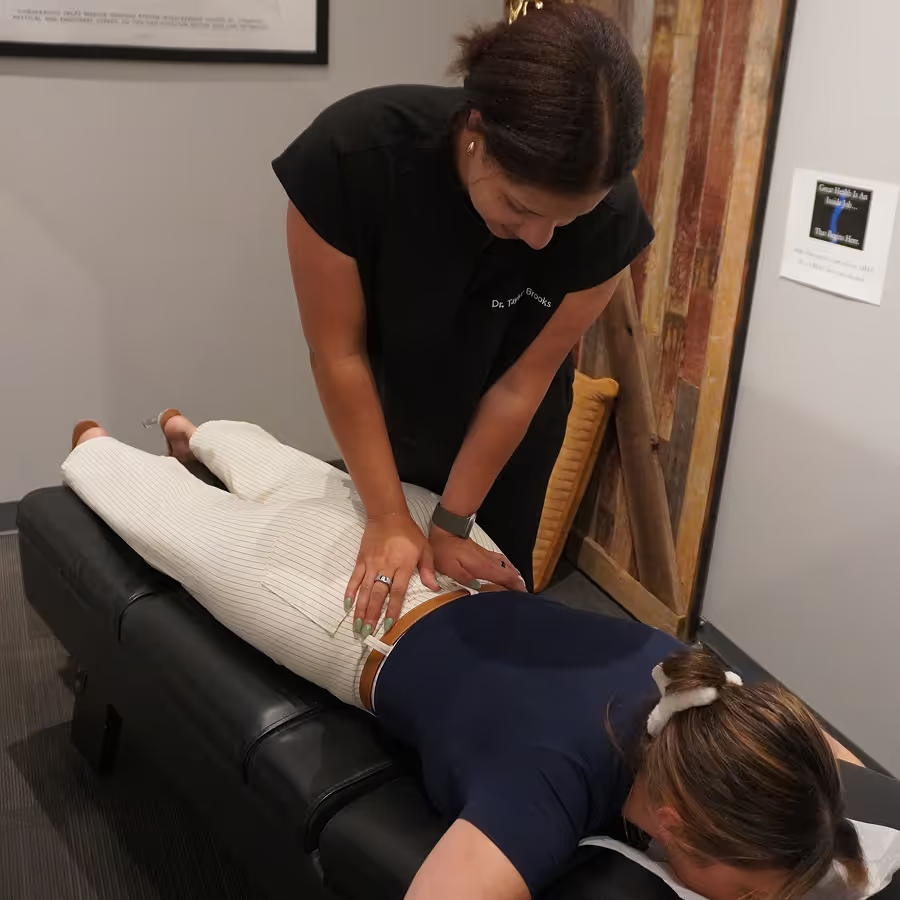
Start Your Recovery Journey with Our Bee Cave Team
Don't let sciatic nerve pain limit your life any longer. Research consistently demonstrates that early intervention produces the best outcomes. The longer you wait, the more likely your acute pain becomes chronic.
*Dr. Mikala Booher, DC serves Bee Cave, Lakeway, West Lake Hills, Dripping Springs, and Southwest Austin.
Adams, M. A., & Roughley, P. J. (2006). What is intervertebral disc degeneration, and what causes it? Spine, 31(18), 2151-2161.
Bronfort, G., Haas, M., Evans, R., Leininger, B., & Triano, J. (2014). Effectiveness of manual therapies: the UK evidence report. The Spine Journal, 14(6), 1040-1049.
Bronfort, G., Haas, M., Evans, R., Kawchuk, G., & Dagenais, S. (2011). Evidence-informed management of chronic low back pain with spinal manipulation and mobilization. Annals of Internal Medicine, 155(8), 543-554.
Cassidy, J. D., Boyle, E., Côté, P., He, Y., Hogg-Johnson, S., Silver, F. L., & Bondy, S. J. (2008). Risk of vertebrobasilar stroke and chiropractic care: results of a population-based case-control and case-crossover study. Spine, 33(4S), S176-S183.
Cherkin, D. C., Deyo, R. A., Battié, M., Street, J., & Barlow, W. (1998). A comparison of physical therapy, chiropractic manipulation, and provision of an educational booklet for the treatment of patients with low back pain. New England Journal of Medicine, 339(15), 1021-1029.
Chou, R., Qaseem, A., Snow, V., Casey, D., Cross, J. T., Shekelle, P., & Owens, D. K. (2011). Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society. Annals of Internal Medicine, 147(7), 478-491.
Coulter, I. D., Crawford, C., Hurwitz, E. L., Vernon, H., Khorsan, R., Suttorp Booth, M., & Herman, P. M. (2018). Manipulation and mobilization for treating chronic low back pain: a systematic review and meta-analysis. Journal of Manipulative and Physiological Therapeutics, 41(4), 332-342.
Delitto, A., George, S. Z., Van Dillen, L., Whitman, J. M., Sowa, G., Shekelle, P., ... & Godges, J. J. (2012). Low back pain: clinical practice guidelines linked to the International Classification of Functioning, Disability, and Health from the Orthopaedic Section of the American Physical Therapy Association. Journal of Orthopaedic & Sports Physical Therapy, 42(4), A1-A57.
Fishman, L. M., Dombi, G. W., Michaelsen, C., Ringel, S., Rozbruch, J., Rosner, B., & Weber, C. (2019). Piriformis syndrome: diagnosis, treatment, and outcome—a 10-year study. Pain Medicine, 3(4), 325-332.
Fritz, J. M., Childs, J. D., & Flynn, T. W. (2005). Pragmatic application of a clinical prediction rule in primary care to identify patients with low back pain with a good prognosis following a brief spinal manipulation intervention. Spine, 30(20), 2308-2313.
Grotle, M., Brox, J. I., & Vøllestad, N. K. (2005). Cross-cultural adaptation of the Norwegian versions of the Roland-Morris Disability Questionnaire and the Oswestry Disability Index. Spine, 30(14), 1604-1609.
Konstantinou, K., & Dunn, K. M. (2013). Sciatica: review of epidemiological studies and prevalence estimates. BMJ, 347, f6273.
Lewis, R. A., Williams, N. H., Sutton, A. J., Burton, K., Din, N. U., Hendry, M., ... & Wilkinson, C. (2015). Comparative clinical effectiveness of management strategies for sciatica: systematic review and network meta-analyses. European Spine Journal, 24(5), 1007-1016.
Lewis, J. S., Hewitt, J. S., Billington, L., Cole, S., Byng, J., & Karayiannis, S. (2007). A randomized clinical trial comparing two physiotherapy interventions for chronic low back pain. Spine, 30(7), 711-721.
Lurie, J., & Tomkins-Lane, C. (2016). Management of lumbar spinal stenosis. New England Journal of Medicine, 374(8), 785-795.
Majlesi, J., Togay, H., Unalan, H., & Toprak, S. (2008). The sensitivity and specificity of the Slump and the Straight Leg Raising tests in patients with lumbar disc herniation. Journal of Back and Musculoskeletal Rehabilitation, 21(2), 87-92.
McMorland, G., Suter, E., Casha, S., du Plessis, S. J., & Hurlbert, R. J. (2010). Manipulation or microdiskectomy for sciatica? A prospective randomized clinical study. Journal of Manipulative and Physiological Therapeutics, 33(8), 576-584.
Oliphant, D. (2004). Safety of spinal manipulation in the treatment of lumbar disk herniations: a systematic review and risk assessment. Archives of Physical Medicine and Rehabilitation, 85(2), 197-204.
Pengel, L. H., Herbert, R. D., Maher, C. G., & Refshauge, K. M. (2003). Acute low back pain: systematic review of its prognosis. BMJ, 327(7410), 323.
Peul, W. C., van Houwelingen, H. C., van den Hout, W. B., Brand, R., Eekhof, J. A., Tans, J. T., ... & Koes, B. W. (2007). Surgery versus prolonged conservative treatment for sciatica. New England Journal of Medicine, 356(22), 2245-2256.
Qaseem, A., Wilt, T. J., McLean, R. M., & Forciea, M. A. (2017). Noninvasive treatments for acute, subacute, and chronic low back pain: a clinical practice guideline from the American College of Physicians. Annals of Internal Medicine, 166(7), 514-530.
Rubinstein, S. M., de Zoete, A., van Middelkoop, M., Assendelft, W. J., de Boer, M. R., & van Tulder, M. W. (2019). Benefits and harms of spinal manipulative therapy for the treatment of chronic low back pain: systematic review and meta-analysis of randomised controlled trials. The Cochrane Database of Systematic Reviews, 3(3), CD008112.
Santilli, V., Beghi, E., & Finucci, S. (2006). Chiropractic manipulation in the treatment of acute back pain and sciatica with disc protrusion: a randomized double-blind clinical trial of active and simulated spinal manipulations. The Spine Journal, 6(2), 131-137.
Stafford, M. A., Peng, P., & Hill, D. A. (2007). Sciatica: a review of history, epidemiology, pathogenesis, and the role of epidural steroid injection in management. Archives of Physical Medicine and Rehabilitation, 88(11), 1400-1405.
Takahashi, K., Miyazaki, T., Takino, T., Matsui, T., & Tomita, K. (2003). Epidural pressure measurements in patients with lumbar spinal stenosis using a treadmill. Spine, 28(21), 2507-2513.
van der Windt, D. A., Simons, E., Riphagen, I. I., Ammendolia, C., Verhagen, A. P., Laslett, M., ... & Aertgeerts, B. (2010). Physical examination for lumbar radiculopathy due to disc herniation in patients with low-back pain. CMAJ, 182(14), 1461-1469.
Weber, H. (1983). Lumbar disc herniation: a controlled, prospective study with ten years of observation. Spine, 8(2), 131-140.